
Telehealth isn’t exactly new, but it sure is reaching new heights. And clearly, the reliance on telemedicine surged during America’s recent pandemic. In fact, telehealth use has increased 38X from late 2019 to mid-2021. According to McKinsey, telemedicine is not only growing in popularity among patients of all ages but also being recognized by an increasing percentage of providers as a valuable resource for treating some patients.
To gain a clearer understanding of telehealth trends, we surveyed more than 1,000 people. We asked questions about respondents’ use of telehealth apps, what advantages and disadvantages they’ve found, and what impact telemedicine has had on their healthcare experience.
Spend the next few minutes as we unpack our telehealth findings. The information may surprise you — and encourage you to learn more about telehealth trends and new ways to integrate telemedicine into your practice.

Our respondents were motivated to use telehealth apps in different ways. Fifty-three percent were first influenced by ads posted on social media platforms, while podcasts persuaded 31% to give their first try with telehealth apps. Interestingly, only 13% of respondents reported first using a telehealth app due to their health insurance plan offering the option. However, 83% of Gen Zers believed employer-sponsored healthcare should include a telemedicine option, as did 69% of respondents overall.
Next we looked into how the use of virtual health services varied across different groups of people by demographics such as age, gender, and location.
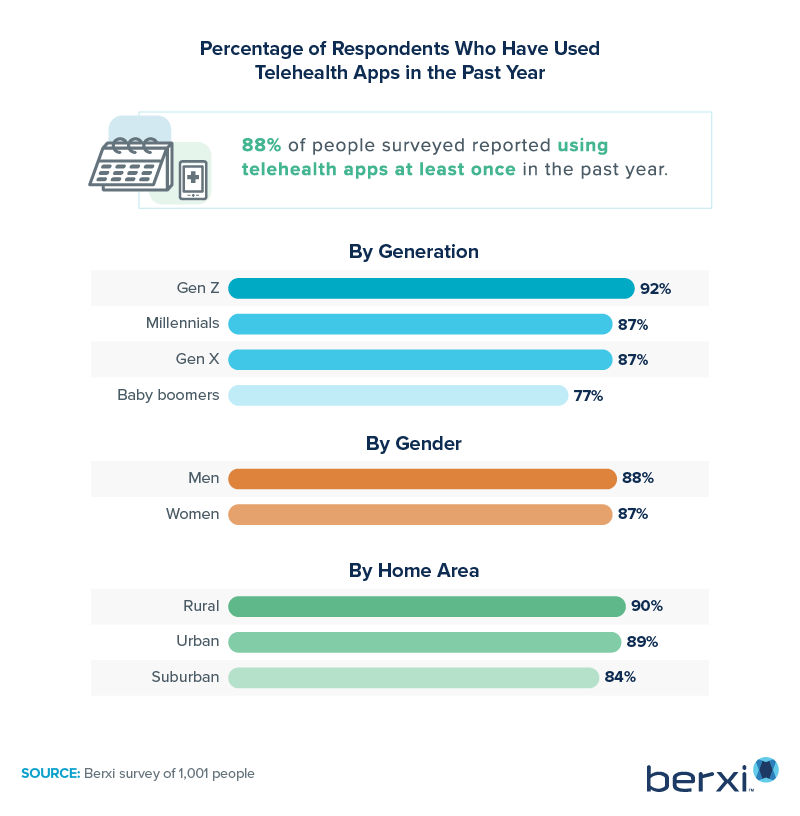
Overall, nearly 9 out of 10 of the people we surveyed reported using telehealth apps at least once in the past year. However, this percentage fluctuated a bit as we broke down telehealth use into groups.
Younger generations were more likely to embrace the use of virtual healthcare than were their older counterparts. Gen Zers were 15 percentage points more likely than baby boomers to report using a telehealth app in the past year. However, when we examined telehealth use by gender, there was only a 1% difference between men and women.
Location proved to affect telehealth app use slightly more than gender. While nearly 9 in 10 respondents living in rural and urban locations reported using a telehealth app in the last year, this percentage dropped off slightly to 84% for those living in suburban areas. People living in rural communities used telemedicine options at a pre-pandemic rate of 82%, versus the 40% of suburbanite respondents who used telehealth visits before early 2020.
When we broke down respondents’ political and social leanings, Democrats were 10 percentage points more likely to use telehealth options than their GOP neighbors.
A 2020 telehealth report from the American Medical Association revealed that 79% of physicians worked in practices that offered telehealth options. In 2018, only one-quarter of doctors worked in a practice where telemedicine was available.
Almost one-third of people surveyed started using telehealth apps during the pandemic. Two telehealth apps stood out in our survey as the most popular: Amazon Care and 4 Your Health. HealthTap, LiveHealth Online, and 98point6 were next, with at least 25% of survey respondents choosing them.
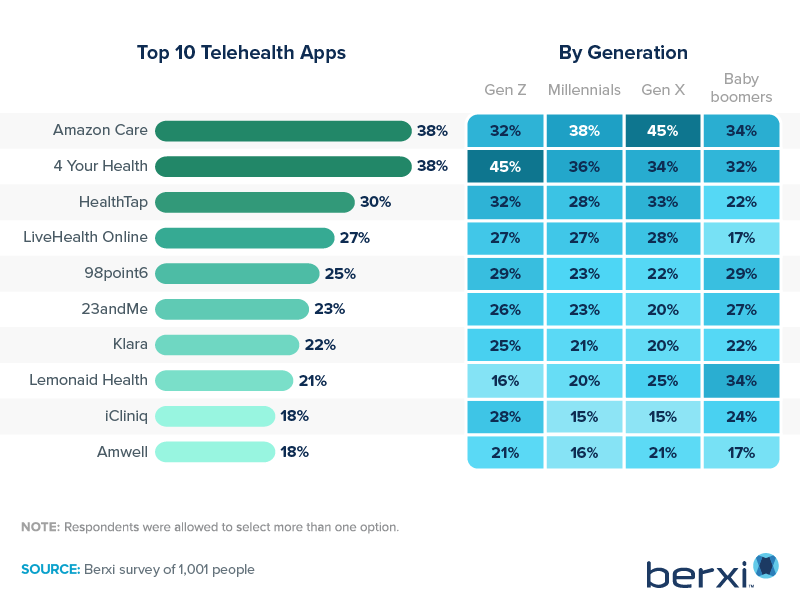
Our survey showed that telemedicine appealed to people across many age groups. More baby boomers preferred Amazon Care, 4 Your Health, and Lemonaid Health, with Gen Xers following a similar pattern but swapping Lemonaid Health for HealthTap. Amazon Care and HealthTap were recommended by physicians most, at 24% and 20%, respectively.
Since the beginning of the pandemic, mental health needs have generated the most use among telehealth users, especially Gen Xers and baby boomers.
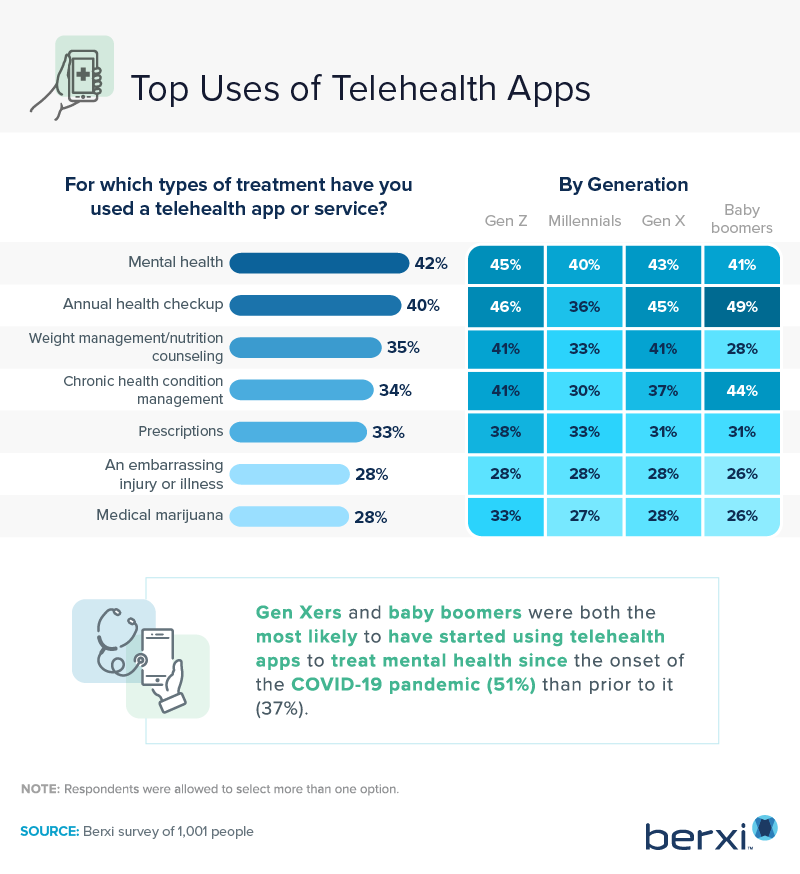
You may think receiving an annual health checkup would require an on-site visit to your healthcare provider. However, 40% of survey respondents received a yearly checkup via a telehealth option. Another 35% sought remote weight management and nutrition counseling.
Survey respondents seeking mental health services preferred a combination of in-person and telehealth visits. When asked about preferences for receiving annual health checkups, 45% preferred a telehealth option, compared to 27% who preferred an in-person exam.
Patients managing chronic or long-term healthcare needs were nearly evenly split in their preferences, with roughly one-third preferring telehealth, in-person visits, or a combination of the two. Those wanting to control their weight or seeking nutrition counseling as well as those with prescriptions were also pretty evenly divided on which option they preferred.
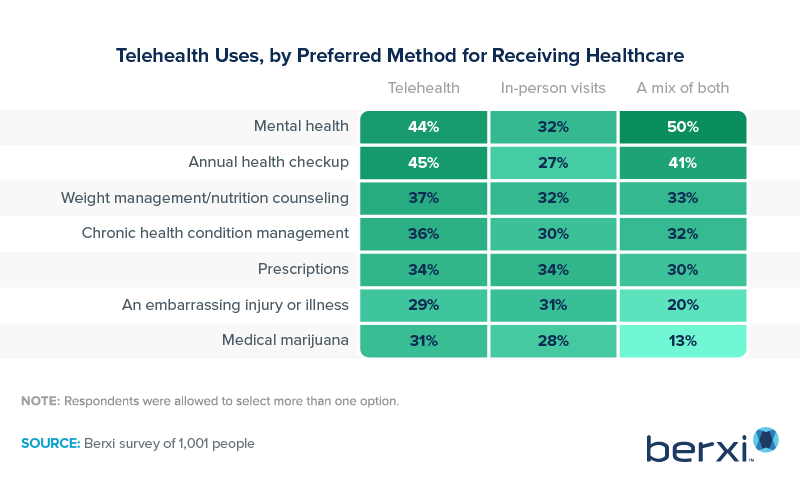
Another interesting finding is that 31% of survey respondents said they preferred to handle their medical marijuana needs via telehealth. Medical marijuana is now legal in almost three-quarters of U.S. states, and during the pandemic, many of those states issued temporary emergency orders that allowed patients to seek prescriptions or advice for medical cannabis usage via telehealth. Although some states have now revoked the use of telehealth for medical marijuana patients, others have extended these provisions into 2022.
Although telemedicine’s impact on healthcare is still being determined, a majority of respondents (58%) said they prefer telehealth apps when healthcare needs arise. Slightly over one-quarter opted for in-person visits, and 15% liked a hybrid of telemedicine and on-site visits.
Patients identified a number of benefits from using telehealth, with the most obvious being saved time. Driving to a healthcare provider’s office and sitting in a crowded waiting area can certainly eat up a chunk of the day. And that’s not even accounting for the time it takes to find a parking space.
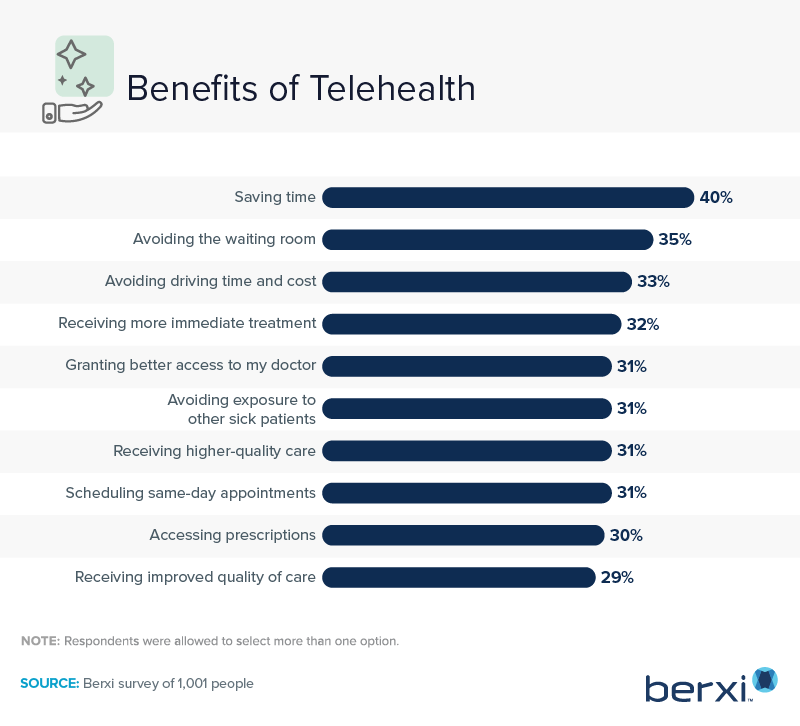
In addition to saving time, 35% of respondents appreciated not sitting around in a healthcare provider’s waiting room. Receiving more immediate treatment, avoiding potential exposure from other patients, and having better access to providers were other benefits identified by survey respondents.
Patients obviously liked the convenience and comfort factors, as demonstrated in this survey. And technology advancements will enable providers to connect with patients even more effectively. In fact, one recent tech breakthrough allows vital measurements such as blood pressure, resting heart rate, and weight to be recorded remotely and submitted directly to a provider’s office.
Another advantage of telemedicine is that it allows more than one provider to meet with a patient at the same time. For example, an internist in Boston and a cardiologist in Los Angeles could meet with their Chicago-based patient all in one appointment. Until the advent of telemedicine, such an involved exchange was impossible.
Time and out-of-pocket costs remain essential elements when using telehealth services. Another important element to consider is not driving to the doctor’s office or waiting. Before the pandemic, Americans spent 34 minutes on average traveling to doctor appointments and 11 minutes waiting to be seen once they got there. According to our respondents, the average time for a telehealth visit was 26 minutes, compared to 31 minutes for an in-person visit. The average out-of-pocket cost for a telehealth consult was about $15 less than seeing a provider personally.
Although these differences might not seem significant, they add up. Over one year, our patients surveyed said they saved an average of $135 and nearly an hour of time by using telehealth rather than in-person visits.
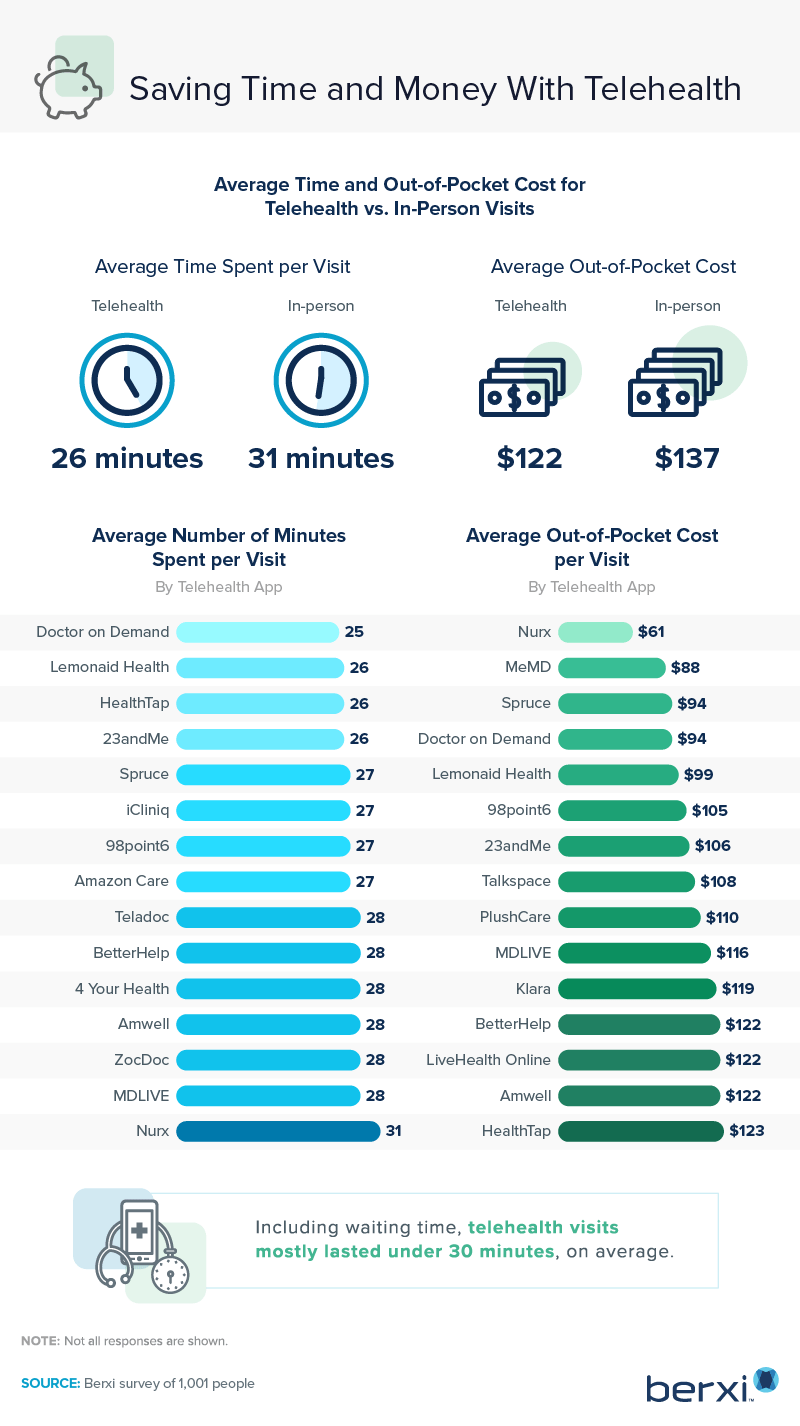
When our respondents ranked telehealth costs per app, Nurx was the least expensive—around $61 per visit. At the other end of the spectrum, four other providers (BetterHelp, LiveHealth Online, Amwell, and HealthTap) charged more than $120 for each telemedicine call.
Even though Nurx was the least expensive, patient visits exceeded 30 minutes, compared to the 25-minute average of Doctor on Demand visits. In fairness to the other telehealth services, the majority of per-visit times ranged from 26 to 28 minutes, which, for most people, is likely acceptable when other considerations, such as drive time and cost, come into play.
What did our respondents view as the main downsides of online provider visits? We asked both those who used the technology and those who didn’t about these perceived cons.
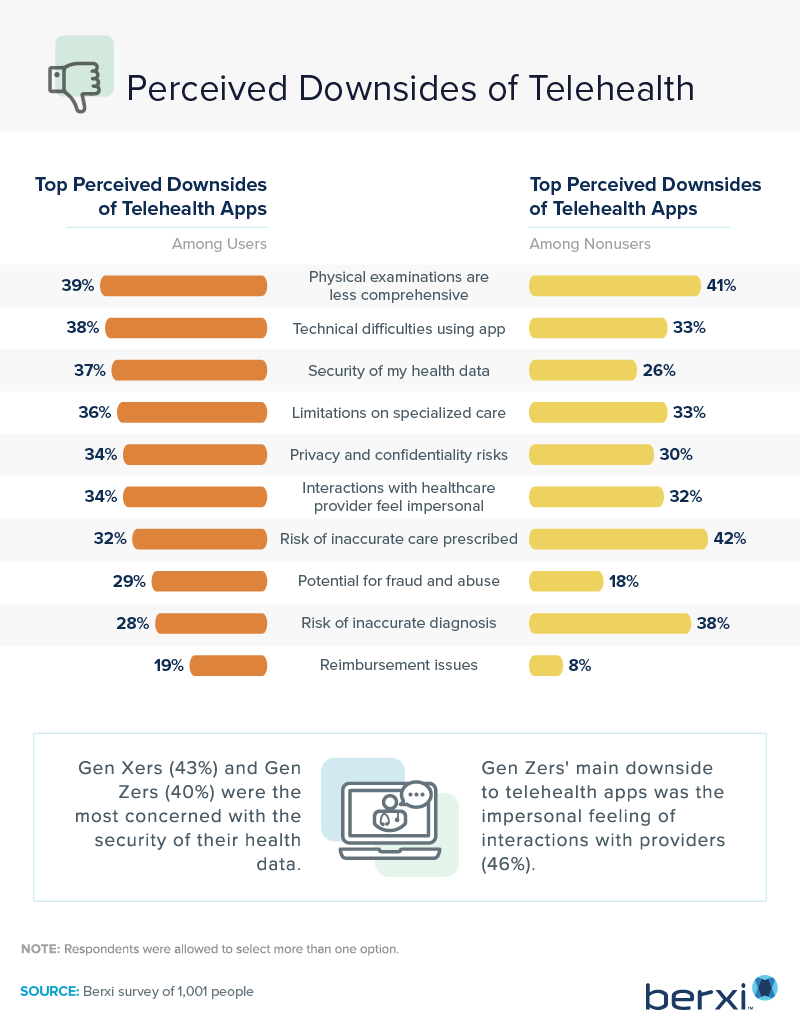
About 4 in 10 respondents in both groups believed that telemedicine physical exams were less comprehensive than in-person ones. Similar percentages of users and nonusers feared technical difficulties when using telehealth apps and had privacy concerns.
A provider’s “bedside manner,” or how they interact with patients during a healthcare exam, has long been a vital issue in healthcare. A provider’s bedside manner is especially important during the world’s recent pandemic. Thirty-four percent of telehealth app users reported that telehealth visits can feel impersonal. Respondents also expressed concern about the possibility of being misdiagnosed during a telemedicine session.
Data security represents one of the more significant concerns expressed by telehealth users. Just under 30% of users, compared to 18% of nonusers, were concerned about potential fraud and abuse when accessing telehealth services. Although protected by many federal laws, such as HIPAA (Health Insurance Portability and Accountability Act), the overall security of patient records remained a concern for 37% of telehealth app users.
As with any medical practice, there are risks involved with providing telehealth services, some of which are unique to telehealth. With the speed at which some practitioners are adding telehealth to their repertoire, it’s important to make sure your risk management policies and procedures are evolving at the same rate. (See A Healthcare Provider’s Guide to the Most Common Telehealth Risks.)
Also be sure to check that your malpractice insurance policy is up to date and covers telehealth. (If you’re interested in getting a quote from us, please go here.)
While telemedicine’s advantages are numerous, in-person healthcare visits will probably never completely vanish. Patients sometimes prefer them, and procedures like imaging tests and blood draws still require an in-person visit. And since insurance companies ultimately decide what is and isn’t covered, both patients and providers may be limited in who can access and utilize telehealth options.
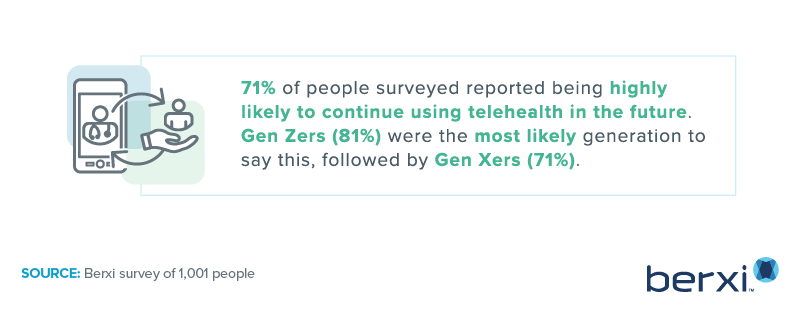
That said, with 71% of Americans planning to use telehealth in the future and 58% saying they prefer virtual to in-person appointments, there’s no question that advancements in telemedicine will continue — along with the number of providers adding virtual services, even if just for follow-up visits.
We surveyed 1,001 people from November 23–29, 2021, to get their sentiments on telehealth apps. 876 respondents used telehealth services in the past year, and 127 did not. Among them, 59% identify as men, and 41% as women. Respondents were asked for their birth year and were organized by generation accordingly: Baby boomers (born 1946–1964), Generation X (born 1965–1980), Millennials (born 1981–1997), and Generation Z (born 1998–2017).
For generation breakdowns, sample sizes were as follows:
For short, open-ended questions, outliers were removed.
To help ensure that all respondents took our survey seriously, they were required to identify and correctly answer an attention-check question.
Survey data have certain limitations related to self-reporting. These limitations include telescoping, exaggeration, and selective memory. We didn’t weight our data or statistically test our hypothesis. The margin of error was +/- 3% with 95% confidence interval.
The American healthcare marketplace continues to grow, and providing valuable information to consumers is vital. As long as it’s for noncommercial purposes, we’re more than happy for you to share this information with your readers. Our only request is that you link back to this page and give the appropriate credit where it’s due.
Last updated on Jul 24, 2024.
Originally published on Mar 31, 2022.
More:
The views expressed in this article are those of the author and do not necessarily reflect those of Berxi™ or Berkshire Hathaway Specialty Insurance Company. This article (subject to change without notice) is for informational purposes only, and does not constitute professional advice. Click here to read our full disclaimer
The product descriptions provided here are only brief summaries and may be changed without notice. The full coverage terms and details, including limitations and exclusions, are contained in the insurance policy. If you have questions about coverage available under our plans, please review the policy or contact us at 833-242-3794 or support@berxi.com. “20% savings” is based on industry pricing averages.
Berxi™ is a part of Berkshire Hathaway Specialty Insurance (BHSI). Insurance products are distributed through Berkshire Hathaway Global Insurance Services, California License # 0K09397. BHSI is part of Berkshire Hathaway’s National Indemnity group of insurance companies, consisting of National Indemnity and its affiliates, which hold financial strength ratings of A++ from AM Best and AA+ from Standard & Poor’s. The rating scales can be found at www.ambest.com and www.standardandpoors.com, respectively.
No warranty, guarantee, or representation, either expressed or implied, is made as to the correctness, accuracy, completeness, adequacy, or sufficiency of any representation or information. Any opinions expressed herein are subject to change without notice.
The information on this web site is not intended or implied to be a substitute for professional medical advice, diagnosis or treatment, and does not purport to establish a standard of care under any circumstances. All content, including text, graphics, images and information, contained on or available through this web site is for general information purposes only based upon the information available at the time of presentation, and does not constitute medical, legal, regulatory, compliance, financial, professional, or any other advice.
BHSI makes no representation and assumes no responsibility or liability for the accuracy of information contained on or available through this web site, and such information is subject to change without notice. You are encouraged to consider and confirm any information obtained from or through this web site with other sources, and review all information regarding any medical condition or treatment with your physician or medical care provider. NEVER DISREGARD PROFESSIONAL MEDICAL ADVICE OR DELAY SEEKING MEDICAL TREATMENT BECAUSE OF SOMETHING THAT YOU HAVE READ ON OR ACCESSED THROUGH THIS WEB SITE.
BHSI is not a medical organization, and does not recommend, endorse or make any representation about the efficacy, appropriateness or suitability of any specific tests, products, procedures, treatments, services, opinions, health care providers or other information contained on or available through this web site. BHSI IS NOT RESPONSIBLE FOR, AND EXPRESSLY DISCLAIMS ALL LIABILITY FOR, ANY ADVICE, COURSE OF TREATMENT, DIAGNOSIS OR ANY OTHER SERVICES OR PRODUCTS THAT YOU OBTAIN AFTER REVIEWING THIS WEB SITE.
Click to collapse disclamerWant Berxi articles delivered straight to your inbox? Sign up for our monthly newsletter below!
"*" indicates required fields